The Future of Dental Implants: What to Know About Screwless Solutions
Screwless implant solutions are changing how some clinicians connect implants and replacement teeth, aiming for simpler maintenance and fewer mechanical complications. If you are considering implant treatment in the UK, it helps to understand what “screwless” usually means, how it differs from traditional screw-retained options, and what practical factors—healing time, materials, and costs—tend to influence outcomes.
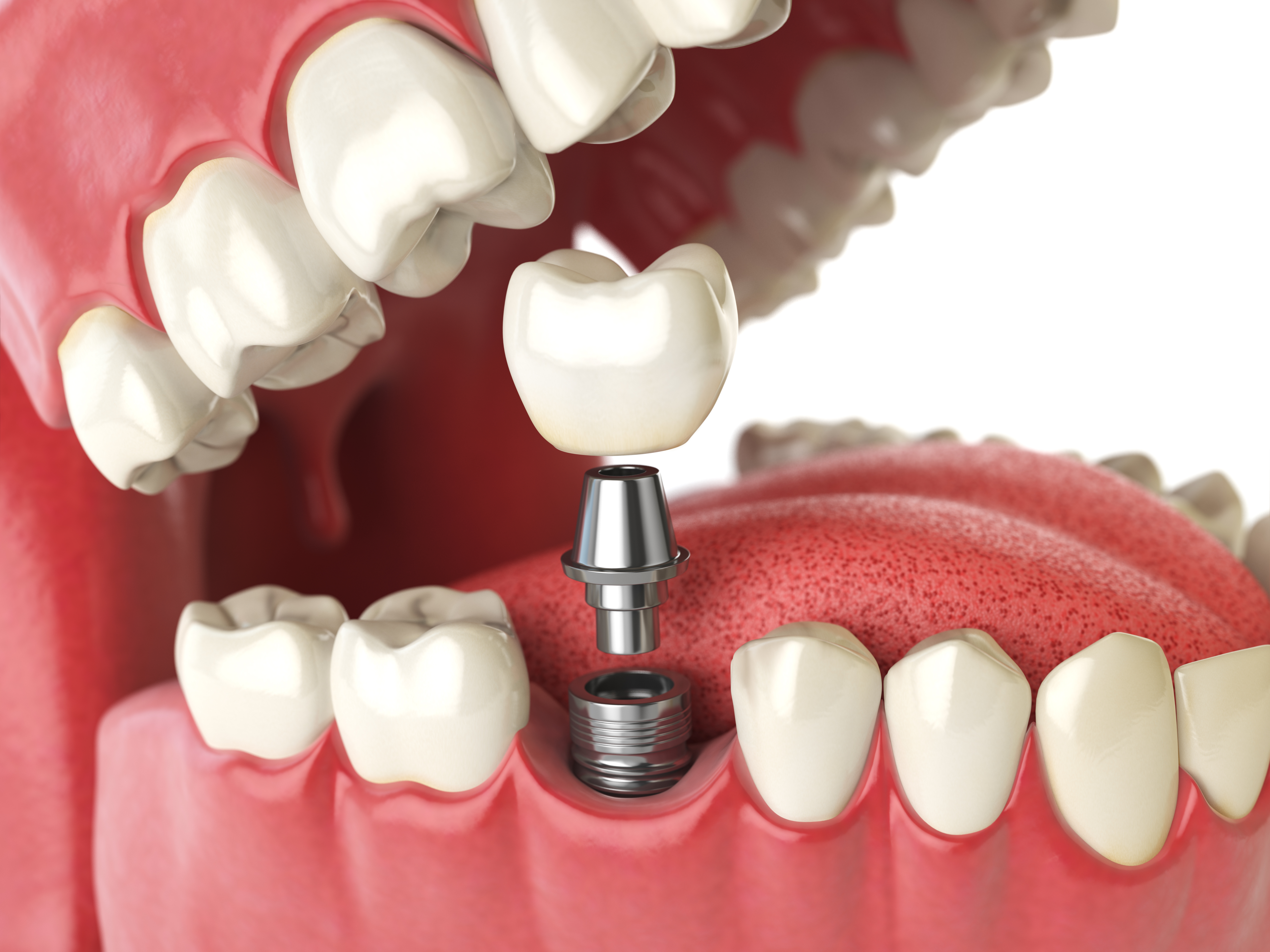
Dental implant treatment has evolved from a relatively standard set of components to a wider range of connection designs, restorative materials, and digital workflows. Among the newer talking points is the idea of a “screwless” solution—typically referring to restorations that are not secured with an access screw through the biting surface. Understanding the terminology, the steps involved, and the real-world trade-offs can help you have a clearer conversation with a UK dental team.
How Dental Implants Work: Traditional vs. Screwless
A dental implant is a small post (commonly titanium or zirconia) placed into the jawbone to support a replacement tooth or teeth. The implant integrates with bone during healing, and then a connector (abutment) supports a crown, bridge, or denture. In traditional screw-retained restorations, a screw fastens the restoration to the implant or abutment, leaving a small access channel that is later filled. In many “screwless” approaches, the restoration is cement-retained or uses a friction-fit/mechanical locking system that avoids a visible screw access hole—though screws may still exist at a deeper level in the system depending on the design.
Steps in the Dental Implant Process: The Screwless Approach
Most implant treatments follow similar clinical stages whether the final tooth is screw-retained or screwless in appearance. First comes assessment: medical history, gum health evaluation, and imaging (often CBCT) to plan implant position and avoid anatomical structures. If bone volume is limited, grafting may be discussed, which can change the timeline.
After placement surgery, a healing phase allows the implant to stabilise. A temporary tooth may be provided in some cases, but immediate loading is not suitable for everyone and depends on bite forces, bone quality, and the clinician’s judgement. Once healed, impressions or digital scans are taken so a lab can fabricate the restoration. With screwless-style restorations, additional attention is often placed on how the crown is seated, how margins are managed, and how the restoration can be retrieved later if maintenance is required.
Factors to Consider Before Getting Implants
Before choosing any implant option, it is worth weighing clinical suitability and long-term maintenance. Smoking, uncontrolled diabetes, gum disease, certain medications, and teeth grinding can affect healing and implant longevity. The position of the implant matters too: back teeth face higher chewing forces, while front teeth place greater emphasis on aesthetics and gum contour.
It also helps to ask how maintenance will work in practice. A key discussion point is retrievability—how easily the crown or bridge can be removed if a component loosens or if cleaning and repair is needed. With some screwless designs (particularly cement-retained crowns), excess cement control and gum health monitoring are important, because cement left under the gum can contribute to inflammation. This article is for informational purposes only and should not be considered medical advice. Please consult a qualified healthcare professional for personalized guidance and treatment.
Modern Trends in Restorative Dentistry: Cost and Accessibility
In the UK, pricing for implant treatment varies widely by region, complexity, materials, and whether extra procedures (extractions, grafting, sinus lift, temporary teeth) are needed. Many quotes are “per tooth” and may or may not include the crown, imaging, sedation, follow-up visits, and hygiene maintenance. As a practical benchmark, a straightforward single-tooth implant with crown in private care is often discussed in the range of roughly £2,000–£3,500, while more complex cases can be higher depending on surgical and restorative needs.
| Product/Service | Provider | Cost Estimation |
|---|---|---|
| Dental implant treatment (private) | Bupa Dental Care (UK clinics) | Typically quoted after assessment; often aligns with UK private market ranges (commonly ~£2,000–£3,500+ per tooth depending on complexity) |
| Dental implant treatment (private) | mydentist (UK practices) | Typically quoted after assessment; costs vary by practice and case (often within common UK private ranges) |
| Dental implant treatment (private) | Portman Dental Care (UK practices) | Typically quoted after assessment; costs vary by location, materials, and need for grafting or sedation |
| Tooth replacement (implant-supported, specialist clinics) | Harley Street dental clinics (London) | Often higher due to central London overheads and specialist provision; case-by-case pricing is common |
| Implant treatment in hospital dentistry (limited pathways) | NHS hospital dental services (via referral) | Not routinely available on demand; eligibility is clinical and pathway-based rather than consumer-priced |
Prices, rates, or cost estimates mentioned in this article are based on the latest available information but may change over time. Independent research is advised before making financial decisions.
Accessibility is also improving through clearer finance options, more widespread digital scanning, and better communication about treatment stages. Even so, “screwless” does not automatically mean cheaper or faster; the main cost drivers are usually clinical complexity, clinician time, laboratory work, and whether additional procedures are required. When comparing quotes, ask what is included (imaging, provisional teeth, abutment type, crown material, aftercare schedule) and how complications or repairs would be handled.
A sensible way to think about the future is that implant dentistry is becoming more personalised: design choices (screw-retained, screwless-looking, or hybrid) are selected around gum health, aesthetics, bite forces, and maintenance strategy rather than a single universal method. For patients, the most helpful next step is often not choosing a buzzword, but clarifying the proposed connection type, cleaning plan, and total cost of ownership over time, including reviews and any likely part replacement.