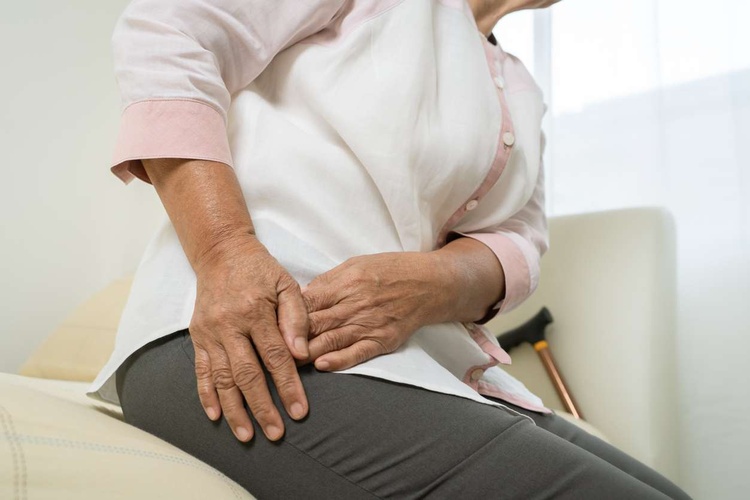
Myelodysplastic Syndrome: Silent Signals You Shouldn’t Ignore
Fatigue that lingers, easy bruising, or frequent infections can look like everyday issues, yet they may reflect changes in how your bone marrow makes blood cells. Myelodysplastic syndrome (MDS) is one condition that can develop quietly, so understanding subtle warning signs and risk factors can help you discuss concerns more clearly with a clinician.
Changes in blood counts can build slowly, and the earliest clues are often dismissed as stress, aging, or a minor illness. Myelodysplastic syndrome (MDS) is a group of disorders in which the bone marrow does not produce healthy blood cells effectively, which can lead to anemia, infections, or bleeding problems over time. Because these effects overlap with common conditions, recognizing patterns and persistence of symptoms matters.
What is Myelodysplastic Syndrome and Who is at Risk?
MDS is a condition where blood-forming stem cells in the bone marrow produce cells that are abnormal, immature, or short-lived. Instead of releasing robust red blood cells, white blood cells, and platelets into circulation, the marrow may release fewer functional cells, leading to cytopenias (low blood counts). In the United States, risk generally increases with age, and many people are diagnosed later in life. Some cases occur after prior chemotherapy or radiation therapy for other cancers (often called therapy-related MDS). Long-term exposure to certain industrial chemicals (such as benzene) has also been associated with increased risk. Less commonly, inherited predispositions can play a role, which may be considered when MDS occurs at younger ages or alongside a strong family history of blood disorders.
What Are the Early Warning Signs of MDS?
Early symptoms often reflect which blood cell line is most affected. Low red blood cells (anemia) can cause persistent fatigue, reduced exercise tolerance, shortness of breath with routine activity, headaches, dizziness, or looking paler than usual. Low white blood cells, especially neutrophils, can show up as more frequent infections, infections that feel unusually severe, or slow recovery from common illnesses. Low platelets can lead to easy bruising, pinpoint red or purple spots on the skin (petechiae), frequent nosebleeds, or bleeding gums. Some people notice these issues only in hindsight, because each symptom alone can seem minor. A common feature is persistence: symptoms that recur, do not match your typical baseline, or gradually worsen over weeks to months.
Why Do These Symptoms Often Go Unnoticed?
MDS can be “silent” because many early changes are nonspecific and easy to rationalize. Tiredness may be blamed on a demanding schedule, sleep problems, depression, or getting older. Bruising can be attributed to thin skin, minor bumps, or blood-thinning medications. Repeated infections may be chalked up to seasonal viruses or exposure to children. Even when symptoms are present, they may fluctuate, which creates false reassurance. Another reason is that mild cytopenias may not produce dramatic symptoms until counts drop further. Sometimes the earliest clue is an abnormal complete blood count (CBC) done for an unrelated reason, such as an annual checkup or pre-operative testing. This is why context is important: a pattern of low counts over time, especially involving more than one blood cell type, is more concerning than a single borderline result.
How Does MDS Affect Your Body’s Blood Production?
Healthy bone marrow works like a factory: it continuously produces red blood cells to carry oxygen, white blood cells to fight infection, and platelets to help blood clot. In MDS, genetic changes in marrow cells can disrupt this process, causing “ineffective hematopoiesis,” meaning the marrow may be busy but still fails to deliver enough healthy cells into circulation. As a result, oxygen delivery can decline (driving anemia symptoms), immune defenses can weaken (raising infection risk), and clotting capacity can drop (increasing bleeding and bruising). Over time, some forms of MDS can progress, and in certain cases the abnormal marrow cells can increase in number and behave more aggressively. Clinicians evaluate this using blood tests, bone marrow studies, and genetic testing to understand subtype and risk, because these details influence monitoring and treatment decisions.
This article is for informational purposes only and should not be considered medical advice. Please consult a qualified healthcare professional for personalized guidance and treatment.
Understanding the subtle, overlapping signals of MDS is less about self-diagnosis and more about noticing persistence and patterns—fatigue that does not resolve, infections that are unusually frequent, or bruising and bleeding that seem out of proportion. Because MDS affects how the body produces and maintains essential blood cells, timely clinical evaluation with appropriate lab work can clarify whether symptoms stem from nutritional issues, medication effects, other medical conditions, or a bone marrow disorder.