Dental Implants in the U.S.: Types, Process, and What to Consider
Tooth restoration procedures represent a significant advancement in modern dentistry, offering a permanent solution for individuals dealing with missing teeth. This guide provides a detailed look at the various types of implants used across the United States, the stages of the surgical process, and the necessary steps for maintaining oral health after the procedure. By understanding these key elements, patients can better navigate their options for achieving a functional and natural-looking smile.
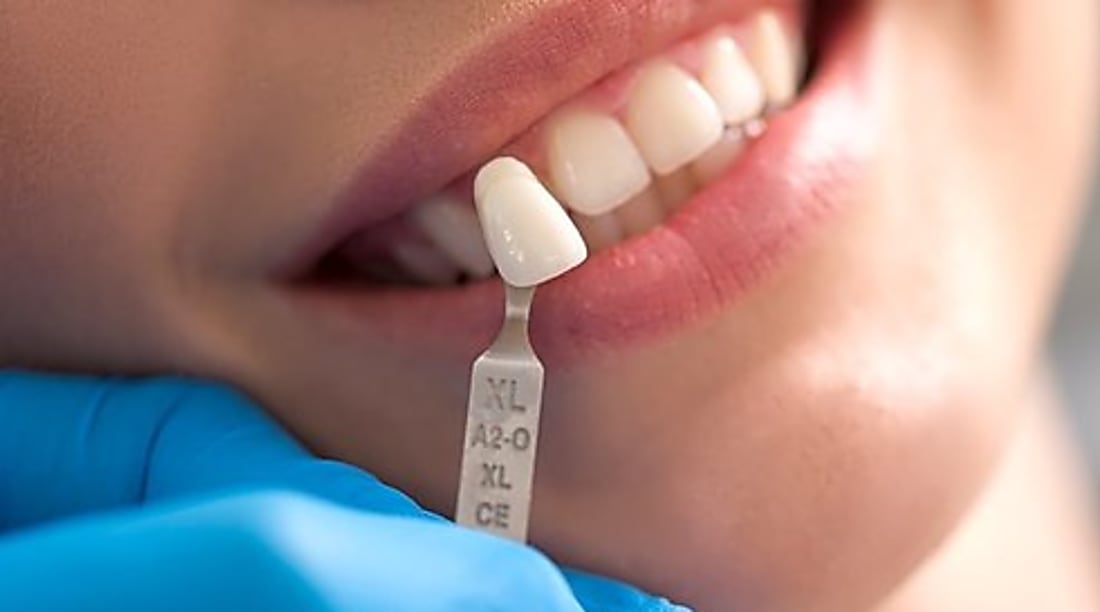
Oral health is a cornerstone of overall physical well-being, yet many adults in the United States face the challenge of tooth loss due to injury, decay, or age-related factors. Beyond the obvious functional difficulties with chewing and speaking, missing teeth can lead to a significant decline in self-confidence and may even cause the remaining teeth to shift or the jawbone to deteriorate over time. Modern restorative techniques have evolved to provide solutions that are not only aesthetically pleasing but also structurally sound, mimicking the natural anatomy of the mouth. One of the most effective methods involves the use of permanent anchors that integrate directly with the jawbone. This approach has transformed how dental professionals address missing teeth, moving away from temporary fixes toward long-term stability and health. Understanding the nuances of these procedures is essential for anyone considering this path to oral restoration.
Dental implant options in the US
When exploring dental implant options in the US, patients will find several techniques tailored to specific anatomical needs and bone conditions. The endosteal variety is the most prevalent, utilizing small titanium posts that act as artificial roots. These are surgically placed into the jawbone and are suitable for most patients who have sufficient bone density to support the hardware. For those with significant bone loss who cannot undergo grafting procedures, subperiosteal alternatives are available. These frames are placed on top of the jawbone but under the gum tissue, providing a stable base for the prosthetic without requiring deep bone integration. Furthermore, full-arch solutions like the All-on-4 technique have gained popularity for their efficiency. This method allows for the replacement of an entire set of teeth using only four strategically angled anchor points, which is often a more viable and less invasive choice for those requiring extensive restoration. Each of these options serves a unique purpose, and a thorough consultation with a specialist is required to determine the most appropriate method for an individual’s specific oral structure and health history.
Treatment process and recovery timeline
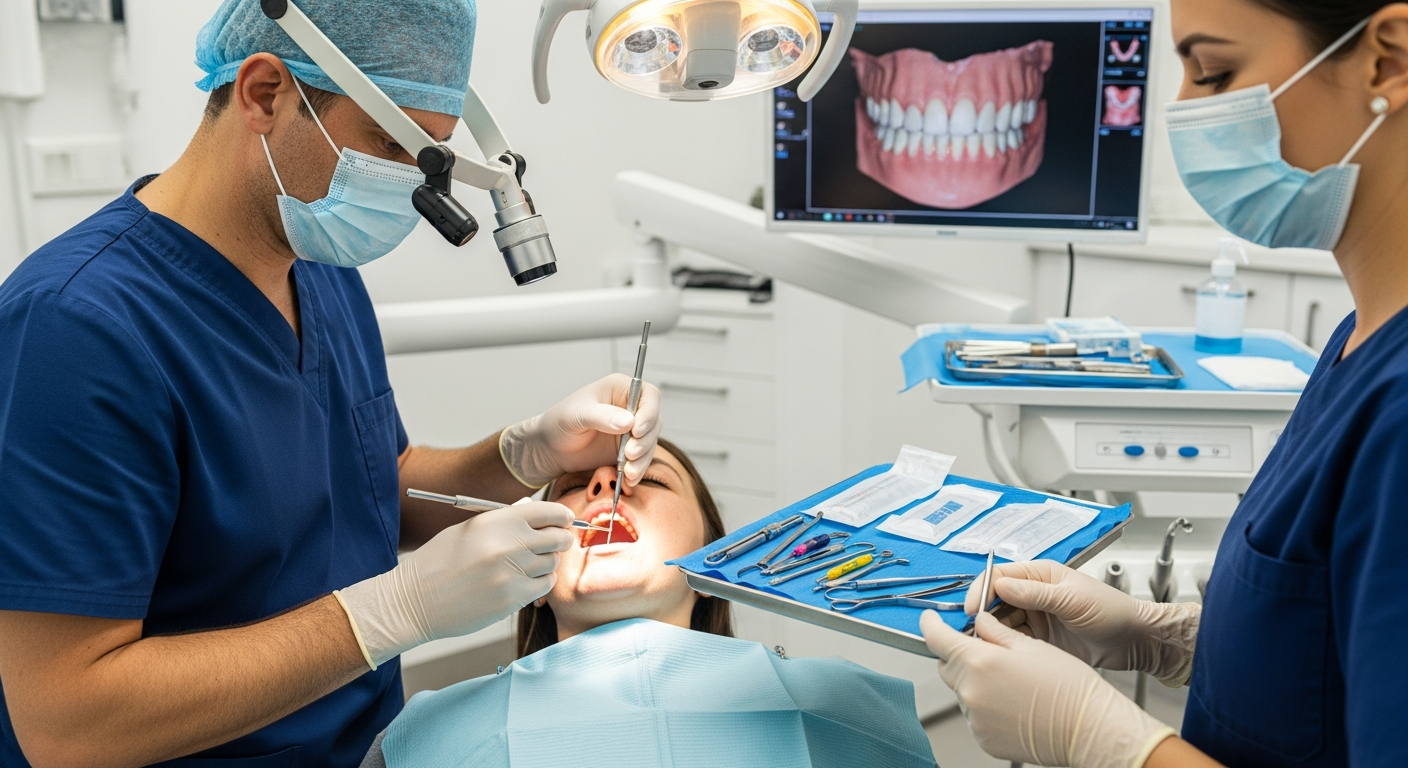
The treatment process and recovery timeline are multi-faceted, often spanning several months to ensure the highest success rate and structural integrity. It begins with a comprehensive diagnostic phase involving digital imaging and 3D scans to map out the bone structure and nerve locations accurately. The surgical phase follows, where the anchor is carefully placed into the bone under local anesthesia or sedation. A critical period known as osseointegration then takes place, lasting anywhere from three to six months. During this time, the jawbone naturally fuses with the titanium surface of the post, creating a bond as strong as a natural tooth root. Once this fusion is complete, a small connector called an abutment is attached to the post. Finally, after the gums have healed around the abutment, a custom-made crown, bridge, or denture is secured on top. While the initial surgical recovery involves only a few days of minor discomfort and swelling, the biological healing process is what dictates the overall duration of the treatment. Patience during this time is vital for ensuring the anchor remains stable and functional for decades to come.
Long-term care and maintenance of dental implants
Ensuring the success of the restoration requires dedicated long-term care and maintenance of dental implants. Although the prosthetic tooth is made of materials that cannot develop cavities, the surrounding gums and bone remain susceptible to infections and inflammation if hygiene is neglected. A condition called peri-implantitis can occur if plaque and bacteria are allowed to build up around the base of the anchor, potentially leading to bone loss and eventual failure of the restoration. Patients are encouraged to use soft-bristled toothbrushes and non-abrasive toothpastes to clean the area without scratching the prosthetic surface. Specialized flossing tools, such as thick floss or water flossers, are also highly recommended to reach the spaces between the prosthetic and the gum line where traditional floss might be less effective. Regular professional cleanings and examinations are essential, as they allow providers to monitor the integrity of the hardware and the health of the supporting tissues, ensuring the restoration remains functional for a lifetime.
In addition to daily hygiene, lifestyle choices play a significant role in the success of restorative procedures. Smoking, for instance, is one of the primary causes of failure because it restricts blood flow to the gums and significantly slows the healing process after surgery. Similarly, individuals with systemic conditions like diabetes or autoimmune disorders must work closely with their medical and dental teams to ensure their health is managed before and after the procedure. Dietary considerations are also important during the initial healing phases; avoiding extremely hard, crunchy, or sticky foods can prevent unnecessary stress on the healing site and the temporary hardware. By adopting a holistic approach to health and following the specific advice of their surgeon, patients can maximize the lifespan of their restorations and enjoy the benefits of improved bite strength, clearer speech, and a more youthful facial structure.
The financial aspect of oral restoration is a major consideration for many families in the United States. Costs can vary widely based on the complexity of the surgery, the materials selected for the crown, and the geographic location of the provider. Some national providers offer standardized pricing models, while private practices may offer more personalized but variable rates.
| Product/Service | Provider | Cost Estimation |
|---|---|---|
| Single Tooth Anchor | Aspen Dental | $3,000 - $4,500 |
| Full Arch Restoration | ClearChoice | $15,000 - $25,000 |
| Endosteal Procedure | Local Periodontist | $3,100 - $5,000 |
| Bone Grafting | Oral Surgery Center | $600 - $2,500 |
Prices, rates, or cost estimates mentioned in this article are based on the latest available information but may change over time. Independent research is advised before making financial decisions.
Choosing to undergo a permanent tooth replacement procedure is a significant decision that impacts one’s quality of life and oral health. By carefully considering the available types of anchors, understanding the commitment required for the healing process, and maintaining a strict hygiene routine, patients can achieve results that last for many years. While the initial investment of time and money is higher than other options like removable dentures, the stability and confidence provided by these modern techniques make them a preferred choice for many. Always seek a consultation with a qualified professional in your area to discuss a personalized treatment plan that addresses your specific needs and goals.
This article is for informational purposes only and should not be considered medical advice. Please consult a qualified healthcare professional for personalized guidance and treatment.